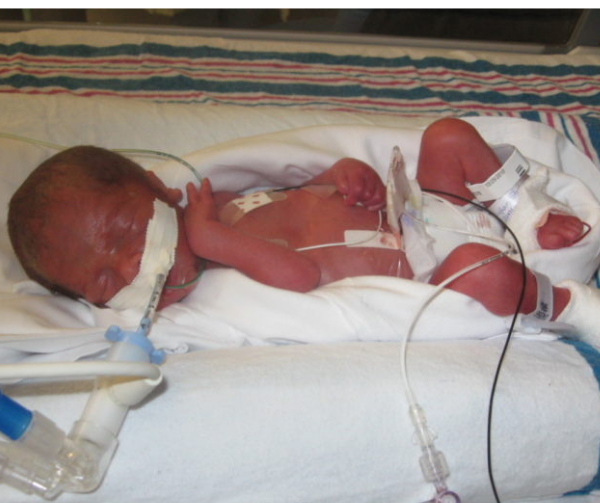
What is Necrotizing Enterocolitis (NEC)?
Predominately due to prematurity, Necrotizing Enterocolitis (NEC) is a rare, inflammatory disease that leads to necrosis (death) of the intestine.
The Morgan Leary Vaughan Fund (Morgan’s Fund) emerged from a need to establish a mechanism for:
- Disseminating credible and timely information about Necrotizing Enterocolitis (NEC) to parents whose infants are most at risk for developing NEC
- Raising the level of public awareness about NEC and the potentially devastating effects it can have on infants and their families
- Advancing research to prevent, diagnose, treat, and ultimately, cure NEC.
Who is Morgan?
Morgan and his twin brother were born at 28 weeks, one day gestation — nearly three months early — each weighing less than 2.5 pounds. At four days old, Morgan developed NEC and lost approximately 20% of his small intestine. Morgan not only survived but also has thrived since his bout with NEC.
Just outside the operating room, the nurse took Morgan out of his incubator. Adjusting his many lines, she extended her arms to present him to me, and said, “Give Mommy a kiss.” I’d spent months anticipating the arrival of my babies, had only been able to visit them a handful of times in their short lives, and hadn’t been allowed to hold Morgan. Feeling awkward and unable to fully grasp all that was happening, I gave him a quick kiss on the forehead. Read More About Morgan.

Speaking of NEC: Unplugged event is a one-day regional conference focused on identifying practical solutions for reducing the devastating effects of NEC on premature infants and their families to be held in Austin, Texas on Monday, March 25, 2019. Event is sponsored by: Prolacta Bioscience and Hand to Hold
Speaking of NEC Unplugged will bring together relevant NEC experts (neonatologists, clinicians, and researchers) and influencers (parents, patient advocates, medical and nursing students, media, and policy makers) to engage and learn from each other’s experiences across the full continuum of NEC; its impact on patients and their parents, the cost to the hospitals that treat it, and the methods to improve both its short and long-term outcomes.
Our overarching goals for the day:
- EDUCATE attendees about NEC and its impact on their community
- SPARK interest in the disease and discussion among attendees
- INSPIRE community engagement and action in the prevention, diagnosis, and treatment of NEC.
Date: Monday, March 25, 2019
Location: Hyatt Place Austin Cedar Park
1315 East New Hope Drive, Cedar Park, TX 78641
There is an amazing line up of speakers with real NEC stories as well as incredibly knowledgeable doctors some of whom include:
- A Neonatologist’s Perspective : Mitch Goldstein, MD, Professor of Pediatrics, Loma Linda University Children’s Hospital; Medical Director, National Coalition for Infant Health
- Surgical NEC : Tory A. Meyer, MD, Pediatric Surgeon, Chairman Pediatrics Leadership Board, Dell Children’s Medical Center of Central Texas
- Improving Human Milk & Breastfeeding Options : Diane L. Spatz, PhD, RN-BC, FAAN, Professor of Perinatal Nursing & Helen M. Shearer Professor of Nutrition, University of Pennsylvania School of Nursing; Nurse Researcher, The Children’s Hospital of Philadelphia (CHOP)
- Short Bowel Syndrome : Muralidhar H. Premkumar, MD, MRCPCH, MS, Associate Director of Intestinal Rehabilitation Services for the NICU, Texas Children’s Hospital
- Speaker Christine Tester – Prevention: A Parent’s Personal Story | Daughter was lost to NEC : My daughter who was born at 28 weeks and weighed 1 lb 11 oz at birth had two bouts of NEC. The first was when she was just over 3 weeks old and she was treated with antibiotics. She was diagnosed again when she was six weeks old. This turned out to be a much more aggressive infection. After an unsuccessful surgery, she was taken off life support. More of her story here: https://handtohold.org/christines-story-of-loss/
- Speaker Kathryn Whitaker – The Disease: A Parent’s Personal Story : Luke Whitaker was born premature at 36 weeks. Before he was born, his parents knew he would only have one working kidney; this is the only thing they knew about Luke before he was born. Luke was growth restricted in utero, so he weighed less than a typical 36 week old baby, weighing 3 1/2 pounds at birth. Luke was admitted to the NICU and when he was nine days old and, and just when his parents thought he’d cleared the hurdle, Luke’s diaper was full of blood. His doctors suspected he had NEC. Luke was then quickly transported from a level 4 NICU to Dell Children’s Hospital. Doctors were recommending surgery, giving him a 2 in 10 chance of surviving surgery. Luke made it through and was readmitted to the NICU, spending 45 days total in hospital NICUs.
To see a full list of schedule, click here. This is a FREE conference to attend – to register check out Morgan’s Fund or Register Here.